Can Heart Failure Be Reversed? Latest Advances and Future Directions
While heart failure isn't fully reversible, recent medical advancements offer hope for improved heart function and quality of life. Learn about the latest treatments, therapies, and research aimed at reversing the effects of heart failure.
DR T S DIDWAL MD (Internal Medicine)
11/3/20248 min read
Heart failure is a serious condition that affects millions of people worldwide. It doesn't mean the heart has stopped working, but rather it's not pumping as efficiently as it should. There are different types of heart failure, and risk factors include high blood pressure, coronary artery disease, diabetes, and obesity. Doctors can diagnose heart failure through various tests, and medications are a cornerstone of treatment. There are four main medication classes used: ACE inhibitors/ARBs, beta-blockers, mineralocorticoid receptor antagonists, and SGLT2 Inhibitors. Each works in different ways to improve heart function. Diuretics and other medications may also be prescribed depending on the individual's condition. Besides medications, lifestyle changes are crucial for managing heart failure. This includes a healthy diet, regular exercise, weight management, and stress reduction. In severe cases, advanced treatments like device therapy or surgery may be needed.
The future of heart failure treatment is promising with new medications, devices, and surgical techniques under development. Early detection, proper treatment, and a healthy lifestyle can help people with heart failure live long and fulfilling lives.
Heart Failure in 2024: A Comprehensive Guide for Patients and Caregivers
Heart failure affects millions of people worldwide and represents one of the most significant challenges in modern cardiology. Despite its ominous name, heart failure doesn't mean the heart has "failed" or stopped working—rather, it means the heart isn't pumping as efficiently as it should. In this comprehensive guide, we'll explore everything you need to know about heart failure, from its causes to the latest treatment options available in 2024.
Understanding Heart Failure: The Basics
Heart failure is not a single disease but a clinical syndrome caused by structural or functional abnormalities of the heart. Think of your heart as a pump that's responsible for delivering oxygen-rich blood to every part of your body. When this pump becomes weakened or stiff, it can't meet your body's demands effectively, leading to various symptoms and complications.
The Impact of Heart Failure
Recent statistics paint a sobering picture: nearly 23 million people worldwide are affected by heart failure, and its prevalence is expected to increase by 46% between 2012 and 2030 in the United States alone. This increase is particularly pronounced in the elderly population, making it a critical public health concern.
Types of Heart Failure
Medical professionals classify heart failure based on how well the heart pumps blood, measured by something called the ejection fraction (EF). There are several distinct types:1.
Heart Failure with Reduced Ejection Fraction (HFrEF)
Also known as systolic heart failure
Ejection fraction is 40% or less
The heart muscle becomes weakened and enlarged
Most commonly studied and has more treatment options
2. Heart Failure with Preserved Ejection Fraction (HFpEF)
Also known as diastolic heart failure
Ejection fraction is 50% or higher
The heart muscle becomes stiff and thick
More challenging to treat, often seen in older adults
3. Heart Failure with Mildly Reduced Ejection Fraction (HFmrEF)
A relatively new classification
Ejection fraction falls between 41% and 49%
Represents a "middle ground" between HFrEF and HFpEF
Signs and Symptoms: When to Be Concerned
Heart failure symptoms can be subtle at first but typically progress over time. Key symptoms include:
Common Symptoms
Shortness of breath (dyspnea), especially during physical activity
Fatigue and weakness
Swelling in the legs, ankles, and feet
Rapid or irregular heartbeat
Reduced ability to exercise
Persistent cough or wheezing
Swelling of the abdomen
Rapid weight gain from fluid retention
Difficulty concentrating or decreased alertness
Advanced Symptoms
Severe breathlessness, even at rest
Chest pain if heart failure is caused by heart attack
Fainting episodes
Rapid or irregular pulse
Waking up at night gasping for breath (paroxysmal nocturnal dyspnea)
Risk Factors and Prevention
Understanding risk factors is crucial for prevention and early intervention. The major risk factors include:
Modifiable Risk Factors
1. High Blood Pressure: The leading cause of heart failure
2. Coronary Artery Disease: Narrowed arteries that reduce blood flow
3. Diabetes: Can damage blood vessels and the heart muscle
4. Obesity: Puts extra strain on the heart
5. Smoking: Damages blood vessels and increases heart disease risk
6. Excessive Alcohol Consumption: Can weaken heart muscle
Non-Modifiable Risk Factors
1. Age: Risk increases with age
2. Gender: Men have a higher risk than women
3. Family History: Genetic factors play a role
4. Previous Heart Attack: Damages heart muscle
Diagnosis: How Heart Failure Is Detected
Modern medicine employs various tools and techniques to diagnose heart failure accurately:
Initial Assessment
Detailed medical history
Physical examination
Discussion of symptoms and lifestyle factors
Diagnostic Tests
1. Blood Tests
BNP (B-type natriuretic peptide) levels
Complete blood count
Kidney and liver function tests
Thyroid function tests
2. Imaging Tests
Chest X-ray
Echocardiogram
Cardiac MRI
heart scan
3. Other Tests
Electrocardiogram (ECG)
Stress Test
Cardiac catheterization (in some cases)
Treatment Options: A Multi-Faceted Approach
Heart failure is a serious condition where the heart can't pump enough blood to meet the body's needs. While it can significantly impact quality of life, modern medicine offers a range of effective treatments, including medications. Let's delve deeper into the key medications used to manage heart failure and how they work.
The Four Pillars of Heart Failure Medication
ACE Inhibitors/ARBs/ARNIs:
How they work: These medications work by blocking the renin-angiotensin-aldosterone system (RAAS), which is a hormonal system that regulates blood pressure and fluid balance. By blocking this system, they reduce blood pressure, decrease the workload on the heart, and prevent the heart from enlarging.
Examples: Lisinopril, Enalapril, Valsartan, Sacubitril/Valsartan (Entresto).
Beta-Blockers:
How they work: Beta-blockers block the effects of adrenaline and noradrenaline, hormones that increase heart rate and blood pressure. By blocking these hormones, beta-blockers slow the heart rate, reduce the heart's workload, and improve heart function.
Examples: Carvedilol, Metoprolol.
Mineralocorticoid Receptor Antagonists (MRAs):
How they work: MRAs block the effects of aldosterone, a hormone that causes the kidneys to retain sodium and water. By blocking aldosterone, MRAs reduce fluid retention, lower blood pressure, and protect the heart muscle.
Examples: Spironolactone, Eplerenone.
SGLT2 Inhibitors:
How they work: SGLT2 inhibitors work by blocking a protein called SGLT2, which is responsible for reabsorbing glucose from the kidneys back into the bloodstream. By blocking SGLT2, these medications increase the amount of glucose excreted in the urine, which can help lower blood sugar levels and reduce fluid retention.
Examples: Dapagliflozin, Empagliflozin.
Additional Important Medications
Diuretics: Diuretics, also known as water pills, help remove excess fluid from the body by increasing urine output. This can help reduce symptoms like shortness of breath and swelling.
Ivabradine: Ivabradine works by slowing down the heart rate, which can help reduce the heart's workload and improve symptoms of heart failure.
Vericiguat: Vericiguat is a newer medication that works by increasing the production of nitric oxide, a substance that helps relax blood vessels and improve blood flow to the heart.
Medication Management Tips
Adherence: It's crucial to take medications as prescribed and to not miss doses.
Monitoring: Regular check-ups with your doctor are important to monitor your condition and adjust your medication as needed.
Side Effects: Be aware of potential side effects and report any new or worsening symptoms to your doctor.
Future Directions
New Medications: Ongoing research is exploring new medications that may offer additional benefits for heart failure patients.
Personalized Medicine: The future of heart failure treatment may involve personalized medicine, which tailors treatment to the individual patient's needs.
Gene Therapy: Gene therapy is a promising area of research that may offer new ways to treat heart failure.
2. Lifestyle Modifications
Success in managing heart failure often depends on lifestyle changes:
Diet and Nutrition
Limit sodium intake (usually to 2,000 mg daily)
Monitor fluid intake
Eat a heart-healthy diet rich in:
Fruits and vegetables
Whole grains
Lean proteins
Healthy fats
Physical Activity
Regular, moderate exercise as tolerated
Cardiac rehabilitation programs
Activities appropriate to symptoms and capabilities
Other Lifestyle Changes
Quit smoking
Limit alcohol consumption
Maintain a healthy weight
Manage stress
Get adequate sleep
3. Advanced Treatments
For severe cases, additional interventions may be necessary:
Device Therapy
Implantable Cardioverter-Defibrillators (ICDs): Protect against dangerous heart rhythms
Cardiac Resynchronization Therapy (CRT): Coordinates heart contractions
Left Ventricular Assist Devices (LVADs): Mechanical pumps to support heart function
Surgical Options
Heart valve repair or replacement
Coronary bypass surgery
Heart transplantation (in select cases)
The Role of Artificial Intelligence in Heart Failure Care
An exciting development in heart failure management is the integration of artificial intelligence (AI) and machine learning. These technologies are being used to:
Predict heart failure risk
Detect early warning signs
Optimize treatment plans
Improve patient outcomes
Reduce healthcare costs
Living with Heart Failure: Daily Management
Success in managing heart failure requires active participation in your care:
Daily Monitoring
1. Weight Changes
Weigh yourself daily
Record changes
Report sudden gains
2. Symptom Tracking
Monitor breathing difficulties
Track energy levels
Note any new symptoms
3. Medication Management
Take medications as prescribed
Keep a current medication list
Report side effects
Conclusion
Heart failure is a complex condition that requires comprehensive management and ongoing care. While it presents significant challenges, modern medicine offers more hope than ever before. With proper treatment, lifestyle modifications, and regular medical care, many people with heart failure can lead full and active lives.
The key to success lies in:
Early recognition of symptoms
Prompt medical attention
Adherence to treatment plans
Active participation in self-care
Regular monitoring and follow-up
By understanding your condition and working closely with your healthcare team, you can optimize your treatment outcomes and maintain the best possible quality of life while living with heart failure.
Remember: Heart failure is not a death sentence but a condition that requires careful management. With the right approach and support, you can continue to live a meaningful and fulfilling life while managing this chronic condition.
Faqs
1. What is heart failure? Heart failure is a condition in which the heart can't pump enough blood to meet the body's needs. It doesn't mean the heart has stopped working, but rather that it's not working as efficiently as it should.
2. What are the symptoms of heart failure? Common symptoms include shortness of breath, fatigue, swelling in the legs and ankles, rapid or irregular heartbeat, and reduced exercise tolerance.
3. What causes heart failure? Heart failure can be caused by various factors, including high blood pressure, coronary artery disease, diabetes, obesity, and certain heart conditions.
4. How is heart failure diagnosed? Diagnosis involves a combination of medical history, physical examination, blood tests, and imaging tests like echocardiograms and X-rays.
5. How is heart failure treated? Treatment typically involves a combination of medications, lifestyle changes, and in some cases, advanced therapies like device implantation or surgery. Medications may include diuretics, ACE inhibitors, beta-blockers, and others.
6. Can people with heart failure live a normal life? Yes, many people with heart failure can live normal lives with proper treatment and lifestyle modifications. Regular medical check-ups, medication adherence, and a healthy lifestyle are essential.
7. Is heart failure preventable? While not always preventable, many risk factors for heart failure can be managed. Maintaining a healthy lifestyle, including regular exercise, a balanced diet, and avoiding smoking and excessive alcohol consumption, can
Related Article
Aging and Your Heart: Understanding Cardiovascular Changes Over Time
Journal References
Heidenreich, P., & Sandhu, A. (2024). Advances in management of heart failure. BMJ, e077025. https://doi.org/10.1136/bmj-2023-077025
Sebastian, S. A., Co, E. L., Mahtani, A., Padda, I., Anam, M., Mathew, S. S., Shahzadi, A., Niazi, M., Pawar, S., & Johal, G. (2024). Heart Failure: Recent Advances and Breakthroughs. Disease-A-Month, 70(2), 101634. https://doi.org/10.1016/j.disamonth.2023.101634
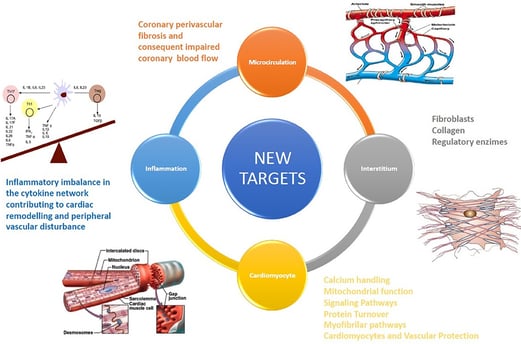
Image credit: https://www.frontiersin.org/files/Articles/665797/fcvm-08-665797-HTML/image_m/fcvm-08-665797-g001.jp
Medical Disclaimer
The information on this website is for informational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health care provider with any questions you may have regarding a medical condition or treatment. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
About the Author:
Dr.T.S. Didwal, MD, is an experienced Internal Medicine Physician with over 30 years of practice. Specializing in internal medicine, he is dedicated to promoting wellness, preventive health, and fitness as core components of patient care. Dr. Didwal’s approach emphasizes the importance of proactive health management, encouraging patients to adopt healthy lifestyles, focus on fitness, and prioritize preventive measures. His expertise includes early detection and treatment of diseases, with a particular focus on preventing chronic conditions before they develop. Through personalized care, he helps patients understand the importance of regular health screenings, proper nutrition, exercise, and stress management in maintaining overall well-being.
With a commitment to improving patient outcomes, Dr. Didwal integrates the latest medical advancements with a compassionate approach. He believes in empowering patients to take control of their health and make informed decisions that support long-term wellness.
